6 a.m.: The smell of tea wafts through the nurses’ station where a dozen women, steaming mugs in hand, are gathered. The handover from the night shift to the day shift on the Neonatology ward starts on schedule. After everyone is updated, Head Nurse Ines Niemann assigns nurses to the different care rooms. There the shift handover continues in smaller teams: from incubator to incubator, from crib to crib.
(Published: December 2016)
The 22 “beds” on the ward are spread over seven rooms, connected by a long corridor painted in a waterworld theme. Vividly patterned fish, corals, boats, lighthouses and beaches bring brightness and color into a place where they sometimes seem to be in short supply. More than 400 babies born prematurely or with illnesses are treated annually in the Neonatology ward at the HELIOS hospital in Schwerin, a northern German city between Hamburg and Berlin. The ward has four Intensive Care rooms, each with space for three incubators, as well as three Intensive Monitoring rooms with four heated beds in each. There are also three “rooming-in” rooms – called ‘Shark,’ ‘Seahorse’ and ‘Whale’ – with two beds each so that mothers can be with their newborns around the clock.
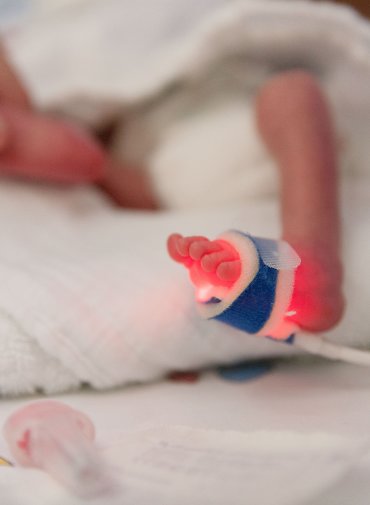
Babies born before the mother’s 37th week of pregnancy are classified as premature but, as Chief Physician Olaf Kannt explains, “not all children born before the 37th week are in the same danger. The more premature the child is, the greater the challenges in treatment and the higher the risk of complications.” Among them: An overburdened intestine and the inability to take nourishment or breathe without assistance.
All of these complications increase the danger of cerebral hemorrhages, Dr. Kannt explains. “Because those are so difficult to treat, we do everything we can to prevent them.” The specific preventive measures to be taken by the staff are included on a special list prepared by HELIOS. In this document, “minimal handling” is the key term in connection with “preemies,” who must always be handled as delicately as possible and only taken from, or placed back in their incubators or heated beds with extreme care.
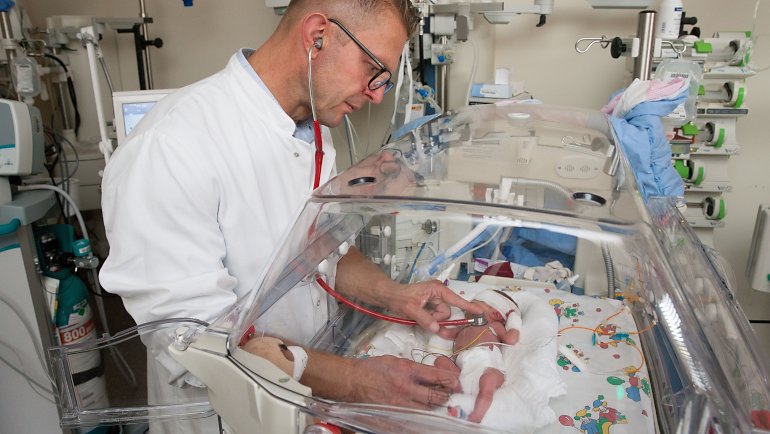
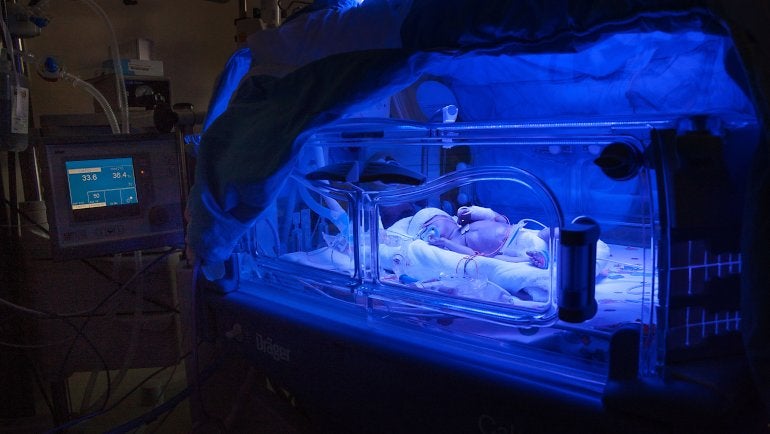
The Intensive Care rooms are kept very warm – about 26 degrees Celsius, or 79 degrees Fahrenheit. Medical devices and hi-tech incubators, along with all the hoses, cables and monitors connected to them dominate the room where Nurse Nicole, 39, is caring for Mattes and Emil. She feeds and changes the twins, who were born when their mother was only 28 weeks pregnant, takes their temperatures and administers their medications. They are also turned over regularly, because pressure sores can easily develop on their highly sensitive skin.
Once every shift, Nurse Nicole measures the babies’ blood pressure, and once a week – today is the day – takes blood samples. “We do that first thing in the morning so that the results are available when the doctors make their morning round,” says the nurse. With a practiced technique she takes gentle hold of a tiny heel, carefully punctures a miniscule hole into it and draws a small quantity of blood into a tube. It will be tested to determine the acid-base balance, which will tell if the infusion therapy needs to be adjusted.

8 a.m.: Dr. Kannt starts the morning round, this time accompanied by an unusually large group of doctors and nurses: Once a week, the Neonatology and Obstetrics teams jointly do the round to discuss the status of the babies in the Neonatology ward. In one of the incubators lies Freja. She was born in the 36th week, so the gestation period is less a concern than the fact that she was born with an intestinal obstruction. As a newborn she had to undergo two operations. Today, the visiting doctors decide Freja’s stitches can be removed.
10 a.m.: The first mothers arrive. One of them is Xenia Dräger, Mattes und Emil’s mother. Ever since she has been allowed to care for her sons, she has been staying in a rooming-in room and from 10 a.m. until midnight washes and changes them, keeps a watchful eye as they sleep, and talks to them. The twins lie in heated, transparent plexiglas incubators, fed through tubes that enter the nose and continue down to the stomach. The room is quiet, except for the peeping from monitors and other assembled medical equipment.During the daytime, parents take the lead in care, with nurses always nearby, ready to advise them or take over if necessary.
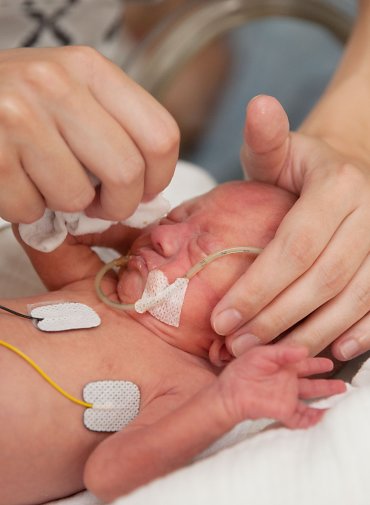
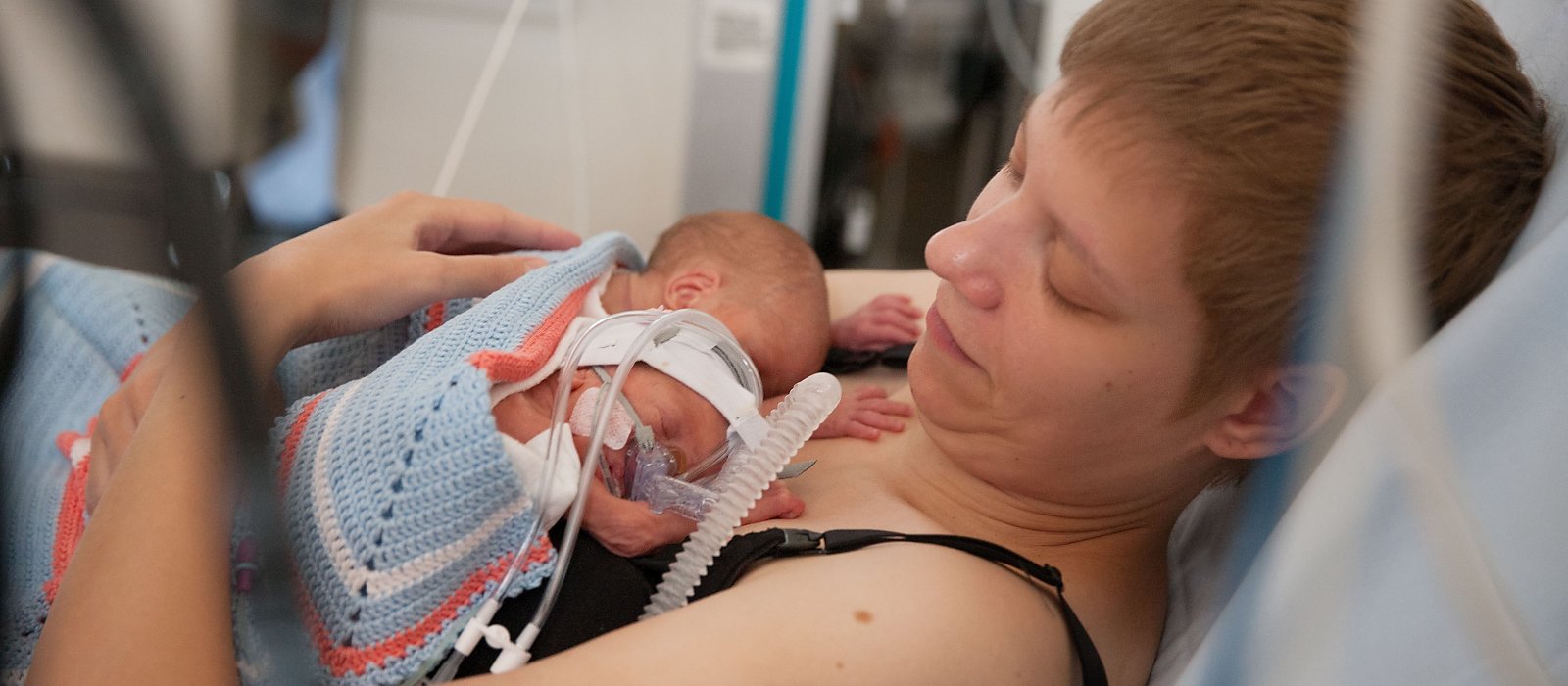
Because their lungs are not yet developed enough for the twins to breathe unassisted, they are attached to respirators. Their tiny faces are almost invisible behind the breathing masks, which make them look almost like miniature skin divers. Electrodes attached to their chests and feet monitor circulation. One suddenly sounds an alarm: Emil’s breathing has been interrupted and his heart rate is dropping. Xenia, who is standing beside the incubator, has been taught by a Neonatology nurse how to respond: she gently massages her son’s chest and presses against his feet. He starts to breathe regularly again, and the monitor goes quiet.
“Mattes does it very nicely, but Emil unfortunately still has frequent interruptions in his breathing,” Xenia says, gently stroking his head. “He still has to learn that.” Twice daily, the twins lay at her breast for one to two hours for so-called “kangarooing.” The term might be humorous, but the practice has a serious purpose: Studies show that it quiets the babies, making both breathing and the heart rate more stable.
2 p.m.: Arriving for the late shift is Nurse Konstanze, who no longer works in the Intensive Care rooms. “Since I became a mother it has been difficult for me to look after the tiny little ones who are struggling for life,” she says. “I feel better here in the Intensive Monitoring rooms.” In these rooms it is the babies’ own rhythms that dictate the care: lying in their warm beds, they are generally monitored only through a small cuff wrapped around a foot.
During the daytime, parents take the lead in care, with nurses always nearby, ready to advise them or take over if necessary. “A lot of parents are nervous dealing with their children, especially when the kids are still sick,” says Nurse Konstanze. “First and foremost, it’s our job to take away that fear, show them how to handle their kids and make them feel secure about it.”

4 p.m.: It’s cuddling time for newborn Freja and her mother, Lisa Dierenfeld, who announces proudly: “She took my breast for the first time today.” There is both joy and relief in the young mother’s voice. “We knew during my pregnancy that Freja had an intestinal obstruction that ended outside of her stomach. We knew that she would have to undergo surgery right after she was born, and be in the ward for premature babies.”
Freja was delivered by caesarean four weeks early, and what followed was also difficult for her mother. “I couldn’t see my baby until two days after her birth,” Lisa recalls. “All the equipment around her bed, the cables and the monitors; it was a shock – I just cried. On the third day I could take Freja in my arms, and that was the first time I really felt like I had given birth.” But the patience and waiting for her daughter to improve have paid off: Lisa will finally be able to move into a rooming-in room later in the day, and she’s full of confidence.
“I am moving in there and I’ll stay until my daughter and I can go home together,” the young mother declares.

8 p.m.: It’s quiet time until 11 p.m., when the next care round will begin. The only sounds on the ward are the low swooshing of the respirators and the occasional alarm signaling that a baby has forgotten to breathe, which sends the nurses rushing in to massage tiny chests or feet until regular breathing starts again. A member of the night shift team is Nurse Janet, who works in the Intensive Monitoring rooms and now has six babies in her care. The 44-year-old nurse does not realize yet that there will be a seventh before the night is out.
10:30 p.m.: The late shift duty doctor, Senior Physician Christian Güttel, arrives and begins checking on what he should expect overnight. He then takes a close look at all the babies, examining some of them, and turns to Nurse Janet. “In the delivery room there’s a woman in her 34th week,” he says. “Don’t be surprised if we get an addition tonight.” It turns out he’s right: The call comes an hour later and, together, doctor and nurse wheel a mobile incubator out of the Neonatal ward and return a short time later with Robin, who is only minutes old.
Dr. Güttel examines the baby boy – the lack of wrinkles under the soles of the feet and the fingernails that don’t yet reach the fingertips are clear signs of a premature birth. “Every child born before the 37th week of pregnancy comes to Neonatology for monitoring,” he says. “With our knowledge and medical equipment we try here to stimulate development as it is in the mother’s womb. Our kids get all the medical help they need.”
3:30 a.m.: The rest of the night is quiet, and already it’s time for the last care round before the shift ends. Nurse Janet draws charts for the day ahead and fills the infusion and disinfectant dispensers. Someone is making tea so that it will be ready when the colleagues from the day shift arrive.
Contact
Helios Kliniken GmbH
Friedrichstr. 136
10117 Berlin
Germany
T +49 30 521 321-0